With all my blog posts, I have endeavoured to be honest, open and authentic with the information I share and this post is no exception. By sharing Mia’s birth, and my experience of being induced, I am not intending to create fear but rather help anyone who finds themselves in a similar situation.
Before I go into the details of Mia’s birth, I want to fill in the gaps between my last post and Mia’s arrival.
10th June (32 weeks and 3 days): The consultant at Stoke Mandeville performs my first amniodrainage and removes 1.2 litres of fluid. This is both a relief (I felt ready to burst – I measured the size of someone who is 38 weeks pregnant) and scary as this procedure could trigger labour, which is not at all ideal at this stage of my pregnancy. Thankfully I am able to stay at the hospital overnight and by the morning the midwives are happy that Pink Peanut is content to stay put…
27th June (34 weeks and 6 days): My last visit to Stoke Mandeville, as all remaining scans before the birth are to be performed at the John Radcliffe in Oxford. I am in touch with the Consultants at the JR weekly and they have told me that I am likely to go into labour any time and if this does not happen, they would like to induce me at 37 weeks. I am not happy with this plan at all as I only want to be induced if either the baby or myself are in danger and it is deemed essential.
10th July (36 weeks and 5 days): I have finally managed to get the consultants to understand my perspective on being induced. Therefore, after a lot of discussions the consultants have agreed to perform a second amniodrainage to give me a chance of going into labour naturally. My second amniodrainage results in 1.6 litres of fluid being removed, and after another overnight stay the midwives are satisfied that Pink Peanut is staying put for now…
17th July (37 weeks and 5 days): Today I have spoken with a female consultant who fully understands my concerns about being induced. However, we have agreed that we can only push things so far. Given that my baby needs special care and surgery soon after she is born, the more controlled the circumstances of when and where I go into labour the better. My induction has been booked in for Monday 29th July. I feel happy with this new plan.
21st July (38 weeks and 2 days): It’s eight days before my planned induction and I am in increasing amounts of pain and discomfort. The UK is experiencing a massive heatwave. I am boiling. Pink Peanut has made it to 38 weeks safely. I make the decision that enough is enough. It’s time to have my baby ASAP!
24th July (38 weeks and 5 days): Induction day
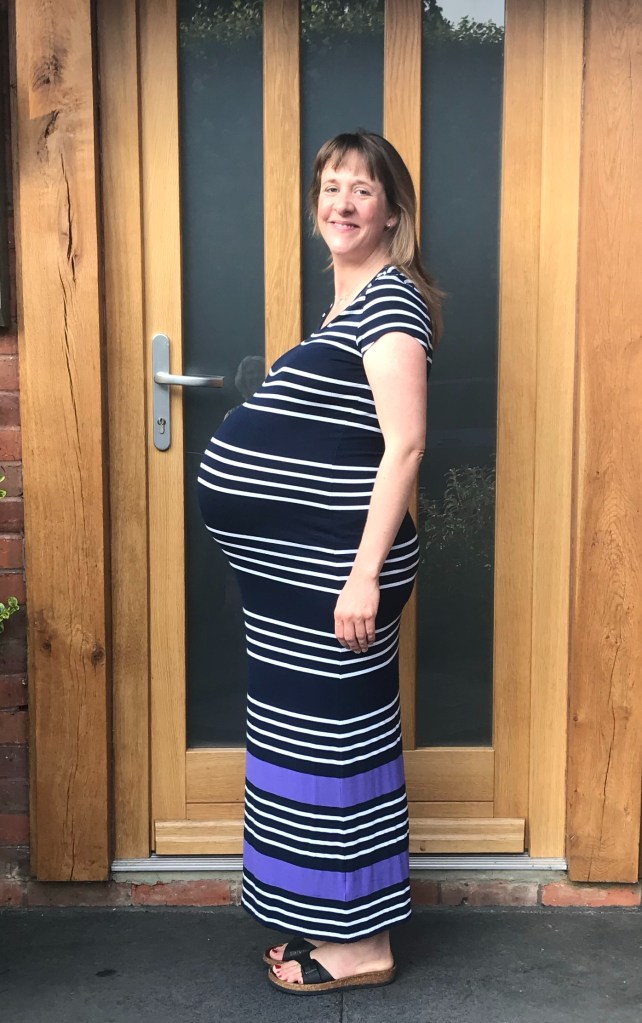
09.00: Sara (my sister), Cheryl (my private midwife who has to act as a Doula in hospital) and I all arrive at the JR in Oxford. Just for fun we get out the tape and measure my bump and discover that I have now reached the size of someone who is 50 weeks pregnant! I feel every inch of it!
The hospital midwife for the first shift is Sophie who I have met before at one of my many trips to Oxford for scans. I immediately feel more at ease as I have my ‘A team’ around me. We are taken to a room in the middle of the corridor with no windows. Today the temperature is due to be at least 32 degrees and there is no air conditioning in the labour ward. The idea, therefore, is that this room will stay much cooler than a room with ‘a view’. Sara quickly starts to make the room look as homely as possible, applying my positive birth affirmations to the wall with Blue Tack and finding suitable spots around the room to place small collections of LED flickering candles.
09.20: My enormous bump is connected to a foetal monitor to check baby’s heart rate. During my pregnancy I have spent quite a lot of time connected to one of these machines so by this stage I feel very at ease and quite in tune with my baby’s normal heart rate rhythm.
10.00: Sophie comes back to see us and confirms all is OK to proceed. I agree to her giving me a ‘sweep’, and at the same time she inserts the induction gel. It feels uncomfortable but not painful and Sophie is able to confirm that I am already 1cm dilated. This is good news considering I was not sure that Pink Peanut was ready to make an appearance any time soon. Maybe I will be meeting my baby today?!
10.10: Another session on the foetal monitor and this time Pink Peanut is very active – it seems she is responding to the interference of her environment.
11.30: I decide it is time for us to go for lunch. We head off from the maternity wing and into the main hospital to take a trip to the M&S café for sandwiches and tea. After lunch we spend a while walking around the hospital during which time I am starting to have mild contractions. These feel strange – some of the surges are stronger than others causing me to pause talking and walking so that I can focus on breathing.
14:00: We arrive back in my room in the maternity wing and settle down to read books and magazines for a bit.
15:00: I have become a bit concerned about the baby’s movements, so I am once again connected to the foetal monitor. Once connected I immediately calm down as I hear the usual rhythmical thud of her heartbeat.
Cheryl suggests that a bit more movement and another trip to the M&S café for tea and cake might be a good idea!
16:15: On the way back to the maternity ward Cheryl encourages me to do some squats on the stairs to help get things moving and, ideally, get my waters to break naturally.

17:00: Sophie is back and wants to examine me again. This time I am 2cm dilated, unfortunately not as much progress as we hoped for. Therefore, the next stage of intervention is proposed, and Cheryl and Sophie agree that my waters should be broken. Unfortunately, we have to wait for a doctor to be present.
18:15: The doctor comes to see me and quickly confirms that Sophie can go ahead and break my waters – also known as Artificial Rupture of Membranes (ARM), or amniotomy. The reason for the procedure is to speed up and strengthen contractions with the aim of shortening the length of labour.
Well, I can tell you it is quite an experience. As previously mentioned, my baby has Oesophageal Atresia (OA), one of the side effects of which is she is unable to process the amniotic fluid in the normal way and this had led to me having polyhydramnios (excess amniotic fluid). Even though we all knew there would be a lot of amniotic fluid no one was prepared for quite how much there is…
Sophie prepares herself for the mini tidal wave heading her way by sitting on a pile of about 20 absorbent sheets. She then uses a crochet-like long-handled hook during her next examination and with a gush the flood gates open very successfully all over the bed, the floor and her phone which she had left in the back pocket of her trousers!
18:45: What a relief, the pressure of all that fluid had been intense for months and within 15 minutes I feel a lot more comfortable. I am now able to balance easily on the birthing ball and have my dinner!
20:00: We bid farewell to Sophie before she hands over to Maddie for the night shift. Maddie and Cheryl agree between them that the next stage of intervention is now needed. I am to be put onto a syntocinon drip, something that none of us wanted for me, however it is the sensible next step given the circumstances
Syntocinon is an artificial form of the natural hormone, oxytocin, and is used to start, or strengthen, contractions for labour. It is given through a drip in your hand or wrist and is started at a slow rate, increasing gradually until you’re having regular contractions at the right strength. Once a syntocinon drip has started, the baby’s heart rate will need to be monitored continuously until delivery.
At this point I am also offered an epidural. It is fairly well known that medically induced contractions are a lot more intense than when you labour naturally and therefore both Cheryl and Sara are strongly advising me to have the epidural as soon as the anaesthetist is available. I am surprised but relieved and quickly agree to this suggestion.
21:00: It now seems like a good time to get settled in for the night. I take the opportunity to have a shower and change into my newly purchased ‘hospital nightie’. I am now ready to rest and hopefully give birth (sooner rather than later)!
21:30: We have just been informed that an anaesthetist is available to come and give me the epidural any moment now. So just before he arrives in the room I have the opportunity to have a last snack of crackers, cream cheese and a shot or two of honey, because once you have the epidural you are advised not to eat until you have given birth. The snack definitely helps me get through what will turn out to be a very long night….
The anaesthetist gives me the epidural which once in place starts to work slowly, and at the same time the syntocinon drip is started. Unfortunately for the first hour of the drip nothing much happens as the cannula is not placed correctly. (Always tricky due to my tiny veins). Once we manage to get the doctor to try and place it again it gets to work and things finally start to progress. The epidural is also doing its job (I have started to lose feeling in the bottom half of my body). Whilst I am able to rest, thanks to a whole host of emotions; nerves, excitement, and fear, I struggle to get much sleep. I have been waiting so long for this moment to arrive and now it is just hours away I can’t really believe it is actually going to happen.
03:00: I am fully awake as I have suddenly got the shakes! Apparently quite normal and I find it very amusing. The drugs have well and truly kicked in!!
06:00: The CTG shows that I am having 4-5 contractions every 10-minutes. I can feel that my left hip is uncomfortable and that something is happening but certainly would not have realised it was anything significant…
06:15: Following an examination it is confirmed that I am fully dilated – wow!
06:45: It is decided that it is time for me to start pushing. Maddie and Cheryl help me onto my right side and I start to push. I am encouraged to use a combination of down breathing (as taught to me by Sara and encouraged by Cheryl,) as well as purple/directed pushing (encouraged by Maddie the hospital midwife).
07:15: The contractions are continuing to come very regularly and with each one, due to the epidural not entirely working on my left hip, I feel a shooting pain. It turns out to be very useful as I know when I need to push. According to Cheryl, Sara and Maddie I am pushing well. I feel like a complete dead weight due to the loss of any feeling in my legs. But the ladies are keen to move me into a better position for pushing and I am helped onto all fours leaning over the head end of the bed, this way we should have gravity working to help us.
07:30: Despite all our best efforts after 15 minutes we are all exhausted! I am therefore helped onto my left side and continue to push for another hour…
08:30: At this stage Maddie is at the end of her shift and hands over to another midwife, Tamara, who comes to join Cheryl, Sara, and me in the room. I have now pushed solidly for two hours. I am not sure how much more of this I can endure! Another registrar performs an examination and Cheryl and Sara’s concerns are confirmed; the baby has moved into an OP position (back to back). Sadly, this means that yet more intervention is proposed in order to ensure that Pink Peanut can be delivered soon and safely into the world.
08:45: I am wheeled out of the cool, dark room where I have spent nearly 24 hours with my trusted birth team and into the bright lights and heat of the day in the corridor. I am taken straight into theatre to be prepared for a trial of forceps and if that does not work then they will quickly need to move and perform a C-section.
To say I am devastated is an under-statement. At this stage the last 24 hours feel like a complete waste of time – why have I had to go through all of this to end up with a C-Section? I am flooded with emotion and exhaustion.
09:00: As my support team are not allowed in with me, I feel so lost, alone and completely out of control. The lights are bright, there are suddenly so many people (my new midwife Tamara, who I met half an hour ago, another anaesthetist, a consultant, the registrar who just examined me, and a team from NICU (Neonatal Intensive care unit) who are on stand-by to take my baby straight off to SCBU (special care baby unit). I feel like no one actually knows me. I am also suddenly in a lot of pain as the epidural has started to wear off, the contractions continue to come thick and fast. I am being instructed not to push and simply to breathe! I am struggling to catch my breath. I literally don’t know how I am supposed to breathe, so all I can do is try and listen to what I am told and wail ‘I want my sister’.
09:30: Finally, after what feels like a lifetime, my wails are answered and Sara is allowed to join me in theatre, unfortunately Cheryl is not. By this stage they have managed to apply the spinal block in preparation for the potential C-Section.
With the threat of a C-Section hanging over us, Sara quickly comes to my rescue, she is calm and focused. The familiarity of her voice and the fact that she is with me allows me to get my breathing back under control. I am then able to summon up all my strength and manage to push through another two contractions and with the help of an episiotomy and the forceps…
09:49: Mia is born!
She is placed onto my stomach, so I am struggling to see her properly. I am scared to touch her, in case I do something wrong. Sara helps me and I touch her head for the first time. She has so much dark hair and such amazing dark brown eyes, I am so pleased she is finally here.

She has to be taken straight over for the NICU team to do a couple of quick checks. They are then happy for us to take a few photos, before she is taken off down the corridor to SCBU with Sara in hot pursuit. I feel devastated at being separated from my baby but somewhat reassured that Sara will be with her – we planned for this in advance.
I have to stay put on my own as there are stitches to be performed. Then I am taken through to a recovery ward to regain the feeling in my legs, before finally being allowed to go and spend some quality time with my daughter.
Whilst this was not the ideal labour, and not the one that I had wished for, throughout my labour, as with my pregnancy, I was well cared for. As I have said previously I am so pleased I had ‘my birth team’ with me throughout. Their support allowed my to feel largely in control throughout these 24 hours of being induced.
I also want to reiterate that this is simply an overview of my experience and is not at all how an induction has to go. Every birth story is different, whether it is straight forward or involves complications. In fact, I know friends who were induced simply to help ease things along towards a straight-forward natural birth. All I would say is make sure you are well supported, don’t be afraid to ask questions and ensure that people are listening, because every woman deserves a positive birth journey.

